Department of Immunobiology, Graduate School of Medicine, Hokkaido University
Ken-ichiro Seino M.D., Ph.D. Immunology
Academic & Professional Experience
- [Education]
-
- 1991 : M.D. University of Tsukuba School of Medicine, Japan
- 1997 : Ph.D. (Medicine) Graduate University, University of Tsukuba
- [Career]
-
- 1991-1993 : Clinical Resident, University Hospital, Tsukuba
- 1995-1999 : Research Fellowship for Young Scientist, JSPS
- 1999-2002 : Lecturer, Dept. Surgery, University of Tsukuba
- 2002-2006 : Researcher, RIKEN Immunology Research Center, Japan
- 2006-2010 : Associate Professor, St. Marianna University
- 2010- : present Professor, Division of Immunobiology, Institute for Genetic Medicine, Hokkaido University
Discovery of methods to enhance the effectiveness of immune checkpoint blockade therapy
 The Department of Immunobiology is engaged in immunological research on transplantation and cancer. In the field of transplantation, research is conducted on the induction of tolerogenic cells from iPS cells, and on cancer, the mechanism of immunosuppression in the cancer microenvironment and new cancer vaccines are being researched.
The Department of Immunobiology is engaged in immunological research on transplantation and cancer. In the field of transplantation, research is conducted on the induction of tolerogenic cells from iPS cells, and on cancer, the mechanism of immunosuppression in the cancer microenvironment and new cancer vaccines are being researched.
Professor Ken-ichiro Seino says, “Immunity is well known to be associated with infectious diseases, and it is known that vaccination can eliminate infectious diseases. It is thought that immunity may have an aggressive effect on cancer as well, but all the mechanisms of cancer have yet to be clarified, and it has become mainstream to think that the relationship between cancer and immunity is complicated.”
Research and development of immunotherapy for cancer began in earnest in the 2000s. Dr. Tasuku Honjo, a distinguished professor at Kyoto University, received the Nobel Prize in Physiology or Medicine in 2018, and the immune checkpoint blockade “nivolumab” (product name: Opdivo®) was developed, making cancer immunotherapy widely known to the world.
“However, much remains to be elucidated. We focus on the relationship between cancer and immunity, especially immune checkpoint blockade (ICB) [1], and are working on research to improve the therapeutic effect of ICB,” Professor Seino says.
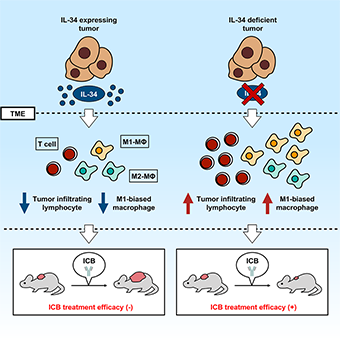
In 2020, a research group led by Professor Seino discovered that a soluble bioactive factor called interleukin 34 (IL-34), which is produced by cancer cells, contributes to the acquisition of resistance to ICB. IL-34 is a soluble bioactive factor first identified in 2008, and its expression in normal humans is known to be limited to the brain and skin. In addition, Professor Seino’s group reported in the past that IL-34 derived from lung cancer cells contributes to the acquisition of resistance to treatment with anticancer drugs. However, the relationship between ICB resistance, which is believed to be present in many types of cancer, and IL-34 remained unclear.
In this study, three types of cancer cells derived from mice were used to clarify that by blocking the expression and action of IL-34, the proportion of inflammatory macrophages, which are said to have anti-tumor effects, and T cells, which are the key to attack on tumor cells, increases in tumors,
thereby improving the therapeutic effect on tumors that were originally resistant to ICB treatment (Figure 1). Therapeutic methods targeting IL-34 are expected to contribute significantly to future cancer treatment because it is believed that the therapeutic effect is further enhanced by combining other treatment methods. The results of this study were the first report to link IL-34 with ICB treatment and were published in the iScience online journal on September 19, 2020.
Development of a transplant model in regenerative medicine and efforts toward cell therapy
 Research on medical transplantation using iPS cells is also a theme that Professor Seino has been working on for many years. iPS cells are expected to be applied to medical transplantation because they can be transformed into various types of cells. However, when iPS cells derived from another person are used for transplantation, the immune cells of the implanted patient may cause rejection as in the case of conventional medical transplantation. To reduce this risk, transplantation is planned using iPS cells that match the patient’s leukocytes to prevent rejection. However, what kinds of immune responses occur – and to what degree – had not been investigated.
Research on medical transplantation using iPS cells is also a theme that Professor Seino has been working on for many years. iPS cells are expected to be applied to medical transplantation because they can be transformed into various types of cells. However, when iPS cells derived from another person are used for transplantation, the immune cells of the implanted patient may cause rejection as in the case of conventional medical transplantation. To reduce this risk, transplantation is planned using iPS cells that match the patient’s leukocytes to prevent rejection. However, what kinds of immune responses occur – and to what degree – had not been investigated.
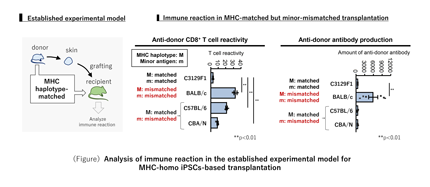
Professor Seino’s group has developed an experimental model of skin grafting in mice using iPS cells, and discovered that even in leukocyte-matched transplantation, T cells react and cause rejection (Figure 2). Furthermore, this model was used to verify the effectiveness of immunosuppressive agents and show that while there are transplant combinations that can suppress rejection over a long period of time, the graft may be rejected even if immunosuppressive agents are used. This result reiterates the importance of controlling the immune response after transplantation. The results of this study were published in Scientific Reports on August 11, 2020.
Recently, the professor has also started research on “cell therapy” as his third line of inquiry. Cell therapy is a method of treating a disease by using the “living cells” of oneself or another person like a medicine. Professor Seino says, “In recent years, not only low-molecular compounds, such as aspirin, but also macromolecules, such as antibodies and proteins, have been used as medicines. Beyond that, there will be treatment by injecting living cells into the body. I felt the potential of cell therapy as a major trend in life science and decided to work on it in earnest as one of the important research themes of the department. Currently, we are conducting joint research with the Department of Gastroenterology and Hepatology and the Department of Gastroenterological Surgery at Hokkaido University on macrophage therapy, which is cell therapy using immune cells, for liver fibrosis, and preparations for clinical trials have begun.”
Cell therapy is a field that is attracting attention as a new treatment method for various diseases, not limited to cancer and transplantation. Professor Seino predicts that cell therapy will become mainstream in the next 20 to 30 years and hopes that students and young researchers belonging to the Department of Immunobiology will enthusiastically engage in cell therapy research, and lead next-generation medical care.


[1] ^ Cancer cells acquire the function of escaping from the immune response by using immune checkpoint molecules in the carcinogenic process. Immune checkpoint blockade therapy (ICB) is a treatment method that blocks the function and activates the immune response.
(Interviewed in August 2021)
A place where students, international students, and researchers from various specialized fields gather

Students who belong to the Department of Immunobiology are from inside and outside Hokkaido University, Sapporo, Hokkaido, and Japan. They come from not only the school of medicine, but also the schools of science, agriculture, engineering and other specialties, and diverse talented students, including international students, inspire one another. Musical instruments, such as guitars, keyboards, and alto saxophones, are kept in the professor’s room, creating an open atmosphere where students play such instruments and talk with the professor. Recently, there have been fewer opportunities for people to gather due to the COVID-19 pandemic, but the openness that allows free interaction between faculty members and students and between senior and junior students remains unchanged.