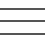Department of Otolaryngology−Head and Neck Surgery, Graduate School of Medicine, Hokkaido University
Akihiro Homma, M.D., Ph.D. Specialized Medicine
- Educational background & professional experience (in sequence of the latest year)
-
- 1983-1989
- M.D., Hokkaido University Graduate School of Medicine
- 1999-
- Assistant Professor, Department of Otolaryngology-Head & Neck Surgery, Hokkaido University Graduate School of Medicine
- 2010-
- Associate Professor, Department of Otolaryngology-Head & Neck Surgery, Hokkaido University Graduate School of Medicine
- 2017-present
- Professor and Chairman, Department of Otolaryngology-Head & Neck Surgery, Faculty of Medicine and Graduate School of Medicine, Hokkaido University
- 2018-present
- Deputy Editor of Auris Nasus Larynx
- Chair of Japanese Clinical Guideline for Head and Neck Cancer
- 2019-present
- Advisor to the Director, Hokkaido University Hospital
Toward the use of superselective intra-arterial chemotherapy as standard therapy

“Those who like to perform surgery can master the art of surgery, while those who like to perform medical therapy can choose a career in internal medicine. We take care of patients with both dizziness and cancer as illnesses that seem totally different but may actually be interrelated as they develop in the same or adjacent organs. What is good about otolaryngology is that it treats such interrelated illnesses in one department,” says Professor Akihiro Homma, who has led the Department of Otolaryngology-Head and Neck Surgery, Graduate School of Medicine, Hokkaido University (established in 1922; hereinafter referred to as the Department of Otolaryngology)since 2017.
The Department of Otolaryngology, which is comprised of five teams – Head and neck, Otology, Rhinology, Voice and Balance – treats a broad array of conditions, including cancers in the head and neck (excluding the brain and eyes) as well as allergies, dizziness, hearing loss, middle ear infections and voice impairment, and conducts both basic and clinical studies of such conditions.

The seventh chairman, Professor Akihiro Homma, who took the position after the fifth chairman, Professor Yukio Inuyama, and the sixth chairman, Professor Satoshi Fukuda, specializes in head and neck cancer. Professor Homma is a leading expert who established the use of superselective intra-arterial cisplatin infusion therapy in the treatment of carcinoma of maxillary sinus, which develops in the nose. The therapy involves the administration of anticancer drugs by inserting catheters selectively into blood vessels through which nutrients are provided to cancer cells (e.g., maxillary arteries branching from the external carotid arteries). Treatment intervals have been reduced successfully through the reduction of side effects by administrating a drug to neutralize anticancer drugs simultaneously with anticancer drug administration. Using this therapy in combination with radiotherapy has also dramatically improved treatment results (Fig. 1).
“Whenever I give presentations on the treatment results of maxillary sinus cancer by superselective intra-arterial cisplatin infusion therapy overseas, I receive great responses. Although multimodal therapy (tripartite treatment) had been provided for head and neck cancer before other types of cancer, there was no treatment that could meet the expectations of patients with inoperative advanced cancer or those who cannot accept surgery due to functional or cosmetic reasons. Mental and physical burdens of patients have been reduced significantly through the introduction of superselective intra-arterial cisplatin infusion therapy that offers a cure without surgery and its use in combination with radiotherapy.”
Professor Homma is currently serving as the leader for multicenter clinical testing conducted jointly with university hospitals and cancer centers throughout the nation to achieve recognition of superselective intra-arterial chemotherapy as standard therapy, and is also holding workshops on the therapy. Professor Homma, who acquired expertise in superselective intra-arterial chemotherapy 20 years ago by corresponding with and directly visiting the American doctor who developed the therapy, is visited by doctors of various specialties from the U.S., where the therapy originated, India and other countries who are seeking advice on the therapy.
“Although there are certain difficulties when it comes to the treatment of head and neck cancer, which must be performed with consideration to organ functions and cosmetic aspects, the ideal treatment is available to patients at Hokkaido University thanks to the high standard of care provided by individual departments,” says Professor Homma. The Department of Otolaryngology has been performing surgery with Plastic Surgery, Neurosurgery, Gastroenterological Surgery and other departments, and has held conferences with the Department of Radiation Oncology every week for the last 50 years. It has also been working closely with the Department of Medical Oncology for more than 10 years, resulting in the practice of ideal team medical care for head and neck cancer.
The department exists for the happiness of all its members.
In the department attracting nationwide attention for a new drug therapy for salivary gland cancer* provided jointly with the Department of Medical Oncology and basic studies, such as the study of human papillomavirus (HPV)-related oropharyngeal cancer*, graduate students are also conducting basic studies on various themes. Dr. Seijiro Hamada (in his second year of the doctoral course) of the Head and neck team is trying to unravel the mechanism behind malignant alteration of oral cancer through the observation of cancer cells using three-dimensional culture, which allows cells to propagate in all directions, and other methods. Another graduate student in the Rhinology team is conducting a study to examine the barrier function of nasal epithelium in hopes of making a breakthrough in finding the cause of eosinophilic paranasal sinusitis, which has increased in recent years but is considered refractory as many aspects of the condition are still unknown.


“Sufficient time is secured for graduate students to concentrate on their studies, and each of them can conduct studies related to the desired treatment group. Instead of staying inside the department, they go to basic medicine departments at the university, in Japan and overseas to pursue their studies, and present their study results at international academic meetings and in English journals. If they work to acquire the ability to read research papers, think logically and give effective presentations during their graduate school years, they will be able to obtain knowledge of other fields and understand the basics of medical science and care. A varied experience like this will contribute greatly to their future clinical practice.”
Itzhak Brook, M.D., MSc, an American doctor who underwent laryngectomy for the treatment of laryngeal cancer wrote about his own experience in “The Laryngectomee Guide” to contribute to improvement in the quality of life of patients facing the same situation. The Japanese version of the book was released in 2019 and made available online. Professor Homma, who supervised the translation of the book by request from Dr. Brook, says, “Dr. Brook’s book about his personal experience, which I had read and been deeply impressed by, remained fresh in my mind, so I wanted to introduce it to Japanese patients.”
Professor Homma’s department is filled with hospitality and always has a peaceful and home-like atmosphere. “The members of the department help each other in everyday treatment even though their specialties vary. Their wishes to study at other universities in Japan and abroad to make progress in their studies and specialties are granted whenever possible. Based on the idea that ‘the department exists for the happiness of all its members,’ I always try to be a supporter for the realization of their dreams.”
(Interviewed in December 2019)
New drug therapy for salivary gland cancer*: drug therapy using a molecular target drug targeted at human epidermal growth factor receptor 2 (HER2), which is associated with the propagation of salivary gland cancer cells.
Study of human papillomavirus (HPV)-related oropharyngeal cancer*: study on the treatment of oropharyngeal cancer caused by HPV infection, which is increasing dramatically around the world.
Shrimp catching event dating back 40 years

There is a unique event in which the medical staff and students go out to Ishikari Beach, a spot popular among sea bathers, to catch shrimp with nets and then return to the department to fry and eat the shrimp with everyone near a barbecue space set up by remaining members. It used to be a tough task for doctors in training to tackle while being tossed by the cold waves in the cold May weather as it was believed that shrimp could only be caught during the cold season. Now, however, everyone enjoys going into the sea in July, as it has recently become known that they can be caught even when the temperature is higher.